Understanding PTSD and Where to Turn for Help
June is PTSD Awareness Month—a time to deepen our understanding of post-traumatic stress disorder (PTSD) and to highlight the network of support available to those who need it most. Whether you’re a veteran, first responder, caregiver, or friend, knowing where to find help can make all the difference on the path to healing.

Professional Treatment Options
The U.S. Department of Veterans Affairs (VA) recommends several evidence-based treatments for PTSD. Many are available through VA Medical Centers, Vet Centers, and telehealth programs. For full details on these therapies, see the VA’s PTSD Treatment page: https://www.mentalhealth.va.gov/ptsd/treatment.asp
1. Trauma-Focused Psychotherapies
- Cognitive Processing Therapy (CPT): A structured, short-term therapy that helps you reframe unhelpful beliefs related to trauma.
- Prolonged Exposure Therapy (PE): Involves gradual, repeated exposure to trauma memories and cues in a safe environment to reduce distress.
- Eye Movement Desensitization and Reprocessing (EMDR): Uses guided eye movements or other bilateral stimulation to process and integrate traumatic memories.
- Cognitive Therapy (CT): Focuses on changing distorted thoughts about the trauma and its aftermath.
Studies show trauma-focused therapies can reduce PTSD symptoms by up to 50% after 8–12 weekly sessions.
2. Medication Management
- SSRIs (e.g., sertraline, paroxetine) and SNRIs (e.g., venlafaxine) are FDA-approved for PTSD and often prescribed as first-line treatment.
- Prazosin may be used off-label to reduce trauma-related nightmares.
- Additional Medications: Atypical antipsychotics or mood stabilizers can be considered for specific symptoms under close medical supervision.
3. Complementary and Integrative Therapies The VA also recognizes the benefit of complementary approaches in a holistic care plan:
- Mindfulness-based stress reduction & meditation
- Yoga and relaxation techniques
- Acupuncture and animal-assisted therapy
Veterans who use integrative therapies in conjunction with standard care report improved sleep quality and reduced anxiety in VA studies.
Peer and Community Support
Connecting with others who share similar experiences provides practical tips and emotional relief.
- VA-Sponsored Support Groups: Free, ongoing peer-led groups at VA centers nationwide. Find a group near you: https://www.mentalhealth.va.gov/ptsd/
- Vet Centers: Confidential counseling and outreach for combat veterans and their families. Search your local Vet Center: https://www.vetcenter.va.gov/
- Nonprofit Organizations: PTSD Foundation of America offers both in-person meetups and online communities dedicated to trauma recovery.
Participants in peer support report a 40% increase in social connectedness and a reduction in feelings of isolation.
Digital and Telehealth Tools
When in-person care isn’t immediately available, digital platforms can fill the gap.
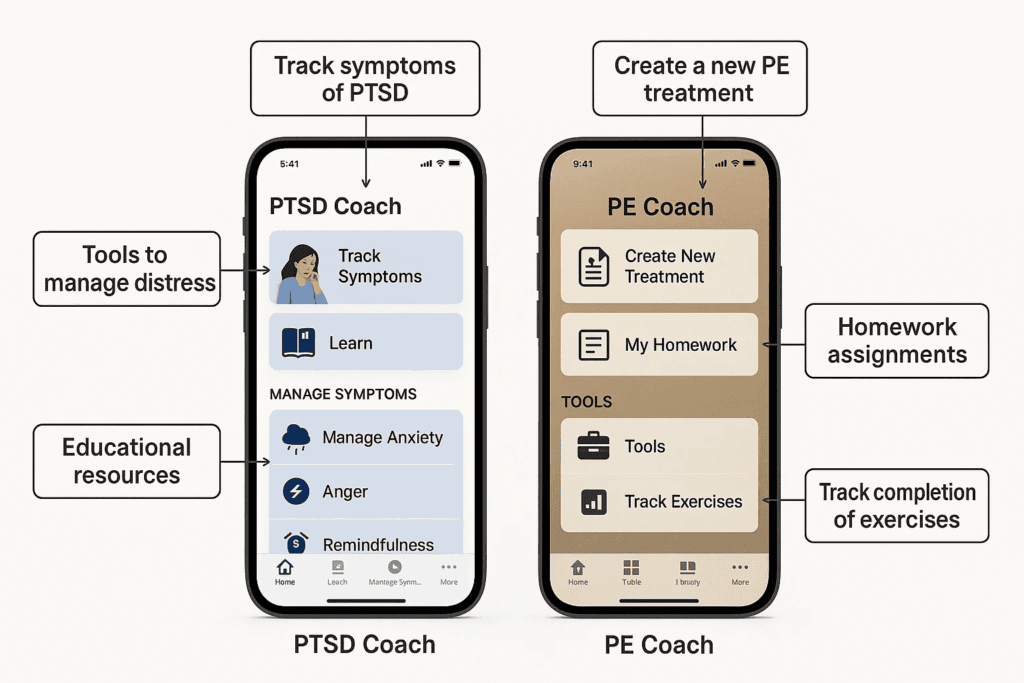
- PTSD Coach App (VA): Free app with symptom trackers, educational tools, and coping exercises. Download here: https://www.ptsd.va.gov/apps/ptsdcoach_app.asp
- PE Coach & CBT-i Coach Apps: Designed to reinforce skills learned in therapy.
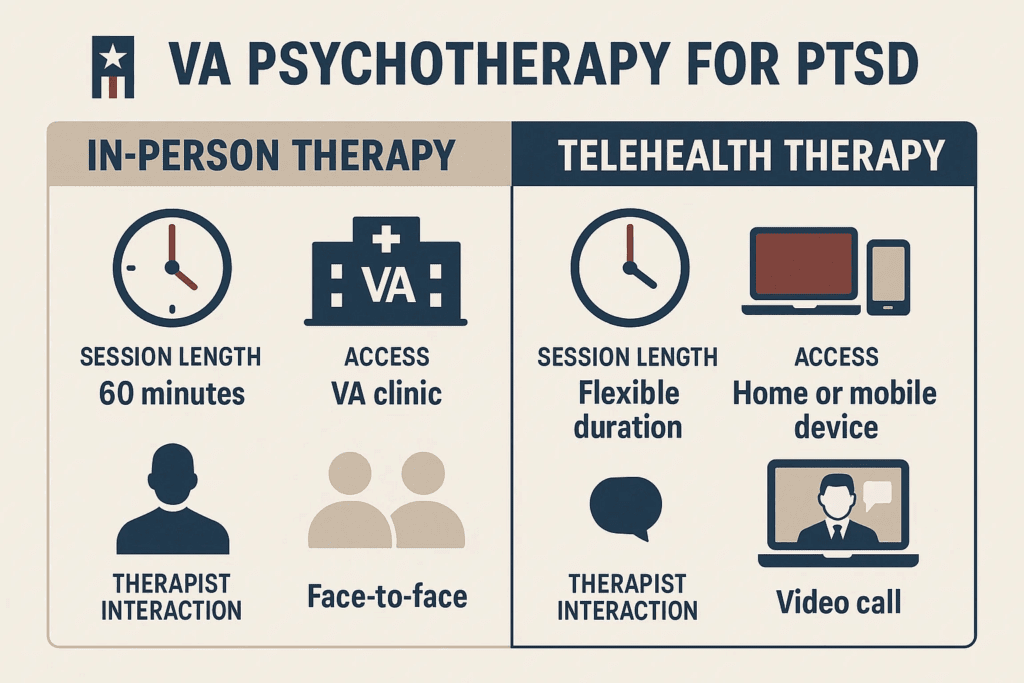
- Telehealth Platforms: VA Video Connect or private services (BetterHelp, Talkspace) connect you to licensed therapists via phone or video.
Self-Help Strategies
Daily practices can help manage symptoms in conjunction with professional care.
- Mindfulness & Breathing Exercises: Short guided sessions to reduce hypervigilance.
- Regular exercise, walking, running, or yoga, can help boost your mood and improve sleep.
- Creative Outlets: Journaling, art, and music therapy offer alternative ways to process emotions.
Engaging in 30 minutes of moderate exercise 3× per week can lower PTSD-related anxiety by 25%.
Resources for Family and Caregivers
Supporting someone with PTSD can be challenging; caregivers need guidance, too.
- Family Therapy: Joint sessions to improve communication and resilience.
- Caregiver Support Groups: Offered through VA and local nonprofits—search at https://www.mentalhealth.va.gov/
- Educational Materials: Downloadable guides from NAMI and the VA’s PTSD site.
Next Steps & Takeaways
- Get assessed: Contact your primary care provider, VA Medical Center, or EAP for a formal PTSD evaluation.
- Explore evidence-based therapies: Visit the VA’s PTSD Treatment page to learn more: https://www.mentalhealth.va.gov/ptsd/treatment.asp.
- Build your support network: Join peer groups and download the PTSD Coach app.
- Integrate self-care: Use daily mindfulness, exercise, and creative strategies to bolster professional treatment.
Seeking help is a sign of strength. You don’t have to face PTSD alone—TNG stands with you, offering expertise, empathy, and actionable resources every step of the way.








